Pain has several possible causes. Pain is an unpleasant sensory and/or emotional experience resulting from actual or potential tissue damage or injury. Sometimes pain occurs without an identifiable physical cause. The purpose of pain is to enable the body to respond and prevent further tissue damage.
You feel pain either a pain stimulus with the sensory nerves and these then transmit signals to the brain. The experience of pain is different for everyone and there are different ways of feeling and describing pain. This makes it difficult to define pain.
Pain can take many forms of expression, for example, stabbing pain, nagging pain, burning pain, etc. Pain can occur acutely (acute pain) or be chronic in nature (chronic pain or chronic pain complaints). Pain can be short term or long term, it can occur at
What is pain?
Alert function
Pain is normally the result of tissue damage. It is part of the body's defense mechanism. It alerts you to take action to prevent further tissue damage. The experience of pain varies. People experience and describe pain differently and this makes it difficult to diagnose. A number of medications and other treatments can help relieve pain. Treatment of pain depends on the cause.
Definition of pain
The International Association for the Study of Pain (IASP) has the following definition of pain:Pain is an unpleasant, sensory and emotional experience associated with actual or potential tissue damage or described in terms of such damage.
Classification of pain
In 1994, the IASP classified pain according to its specific characteristics, in response to the need for a more useful system for describing chronic pain:
- Part of the affected body (e.g., abdomen, lower extremities) where the pain occurs
- System whose dysfunction may cause the pain (e.g., nervous, gastrointestinal);duration and pattern of occurrence
- Intensity and time since inception
- Cause
However, this system has been criticized by professor of neurology Clifford J. Woolf and others as inadequate for the purposes of research and treatment. Woolf proposes three classes of pain:
- Nociceptive pain: caused by active or impending tissue damage leading to activation or excitation of peripheral nociceptors.
- Inflammatory pain associated with tissue damage and immune cell infiltration
- Enpathological pain that is a disease state caused by damage to the nervous system or its abnormal function (e.g., fibromyalgia, peripheral neuropathy (dysfunction of one or more peripheral nerves, where diabetes is the main culprit), tension headache, etc.).
Causes of pain
Pain is felt when special nerves that detect tissue damage send signals to relay information about the damage. These signals travel along the spinal cord to the brain. These nerves are known as nociceptors.
The brain then decides what to do with the pain. For example, if you touch a hot surface, a message will pass through a reflex arc in the spinal cord and cause an immediate contraction of the muscles (called a “reflex”).
This contraction pulls your hand away from the hot surface. This happens so quickly that the message does not even reach the brain. However, the pain message will be transmitted to the brain. Once there, it will cause an unpleasant sensation of pain.
How your brain processes and interprets these signals and the efficiency of the communication channel between the nociceptors or pain receptors and the brain determines how you feel and experience pain. The brain can also release substances, such as dopamine, to counteract the unpleasant effects of pain.
Acute pain and chronic pain conditions
Pain can be acute or chronic.
Acute pain
Acute pain is generally intense and short-lived. It is your body's way of alerting you to an injury or local tissue damage. Treating the underlying injury normally resolves this type of pain. The body's fight-or-flight response is triggered by acute pain, which often leads to a faster heart rate and accelerated breathing.
Different types of acute pain are distinguished:Somatic pain is superficial nociceptive pain felt on the skin or soft tissues just below the skin and is usually clearly localized and sharp, stabbing or throbbing in nature.
Visceral pain is nociceptive pain that originates in the internal organs and lining of cavities in the body.Radiating pain is felt in a different location from the source of tissue damage, such as shoulder pain felt during a heart attack.
Chronic pain
Chronic pain lasts much longer than acute pain. Chronic pain is pain that lasts longer than 3 to 6 months. It often cannot be resolved. The pain can be mild or severe, it can be continuous, as in arthritis, or it can be intermittent, as in migraine. Intermittent pain occurs seizure-like and is absent or only latent between attacks.
The fight-or-flight response eventually stops in chronic pain because the sympathetic nervous system that causes these responses adjusts to the pain stimulus.Breakthrough painChronic pain can usually be treated well with medication. However, short periods of severe pain may occur in this process, which is known as breakthrough pain.
Types of pain
There are also other, more specialized ways to describe pain.
Neuropathic pain
Neuropathic pain (also called nerve pain or neuralgia) follows an injury to the peripheral nerves that connect the brain and spinal cord to the rest of the body. It can take the form of electric shocks, tremors, tingling, numbness (numbness) or other sensations.
Phantom pain
Phantom pain occurs after the amputation of a limb and refers to a pain sensation experienced as coming from an amputated limb.
Central pain
Central pain occurs due to damage in the central nervous system itself. It is often caused by a heart attack, abscess, tumors, degeneration or bleeding in the brain (cerebral hemorrhage) and spinal cord. Central pain can vary
Research and Diagnosis
Interview with the doctor
The diagnosis depends on a person's subjective description of the pain. There is no objective scale for identifying the type of pain, so the doctor will try to find out the nature and intensity of your complaints through an interview. There are several pain questionnaires the doctor can use to diagnose those factors that may have a negative effect on your experience of pain.
In the interview, the doctor will ask, among other things, about:
- Since when you have had the pain symptoms
- The nature of the pain, such as burning, stabbing, or nagging pain
- The location of the pain (or where the pain is felt), how it feels, and how far it feels
- What factors aggravate and relieve the pain
- Whether the pain is constant or intermittent
- The impact of the pain on your daily functioning and state of mind
- The person's understanding of their pain
Measuring pain
For a good assessment and treatment of the pain, it is important to measure and register it regularly. For this, the doctor can use pain scores or pain questionnaires, which provide insight into the severity of the pain and its influence on daily functioning. Sometimes it also helps to fill in a pain diary.
Other indicators of pain
However, when people with cognitive impairment cannot accurately describe their pain, there may be clear indications of the presence of pain. These clues may include:
- Restlessness or agitation
- Crying
- Groaning noises
- Grimacing
- Resistance to care-reduced social interaction
- Increased wandering
- Loss of appetite
- Sleep problems
Treatment of pain
If treatable, the physician will treat the underlying cause of the pain and/or prescribe analgesic treatment, such as medication. When treating pain, the physician follows a step-by-step approach. If there is insufficient pain relief or contraindications, the physician moves to the next step. The doctor starts with paracetamol, then NSAIDs, and then opioids which come in many gradations.
Paracetamol
Paracetamol is an analgesic and fever-reducing drug. It is one of the safest painkillers with relatively few side effects.
NSAID's
Nonsteroidal anti-inflammatory drugs (NSAIDs) are anti-inflammatory drugs that do not belong to the corticosteroid group. Well-known examples are ibuprofen, diclofenac and naproxen. They are suitable for mild to moderate acute pains such as headaches, minor sprains and back pain. NSAIDs can relieve localized inflammation and pain due to swelling. They may cause side effects in the digestive system, including bleeding.
Opioids
Opioids are prescribed for the most extreme acute pains, such as after surgery, burns, cancer and broken bones. Opioids are highly addictive, cause withdrawal symptoms and lose their effectiveness over time.
They require a prescription. In severe trauma and pain situations, the physician will carefully monitor and administer the dose, gradually reducing it to minimize withdrawal symptoms.
Alternatives to medication
A range of non-drug treatments can help relieve pain.
Dry needling
Dry needling is a treatment method to treat painful or tense muscles, which is given by the physical therapist.
Nerve blockade
These injections can numb a group of nerves that acts as a source of pain for a specific limb or body part.
Herbal therapies
There are several herbs that can help a patient deal with pain.
Psychotherapy
Psychotherapy can help with the emotional side of persistent pain. Chronic pain can often affect the enjoyment you derive from everyday activities
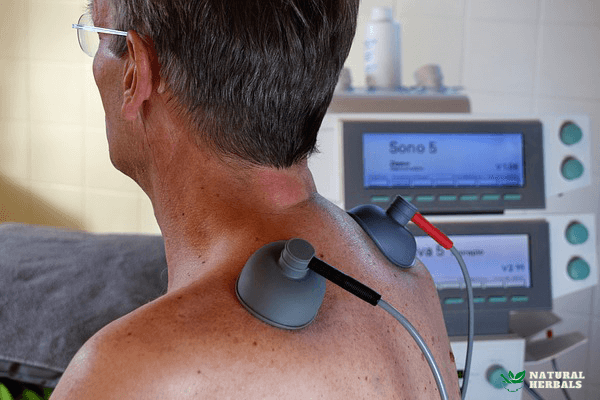
TENS
TENS (transcutaneous electrical neuro stimulation) is a treatment that is done via currents and aims to reduce the opio
Surgery
Several surgeries of the nerves, brain and spine are possible to relieve chronic pain. These include root blockage (Rhizotomy), decompression and Deep Brain Stimulation (DBS or deep brain stimulation).
Biofeedback
Biofeedback is an effective method for learning to relax again in the face of prolonged stress.
Relaxation therapies
This includes a wide range of relaxation techniques and exercises, which can help reduce pain or learn to cope better with pain.
Physiotherapy
A physical therapist can do various treatments to relieve the pain and also do exercises with the patient
Heat and cold
Applying heat and cold therapy can help, depending on the type of injury or pain. Some medications have a warming effect when applied locally to the affected area.
Rest
If the pain is the result of an injury or overuse, rest is the best option.

I am an official member of International Association of Therapists and research natural healing methods and herbs. The posts are my findings.